Understanding Your Path to Recovery
An anorexia rehab center provides specialized, comprehensive treatment for individuals struggling with Anorexia Nervosa, offering various levels of care from 24/7 residential support to outpatient programs. These centers use multidisciplinary teams—including therapists, physicians, dieticians, and nurses—to address the physical, psychological, and nutritional aspects of recovery through evidence-based therapies, medical monitoring, and individualized treatment plans.
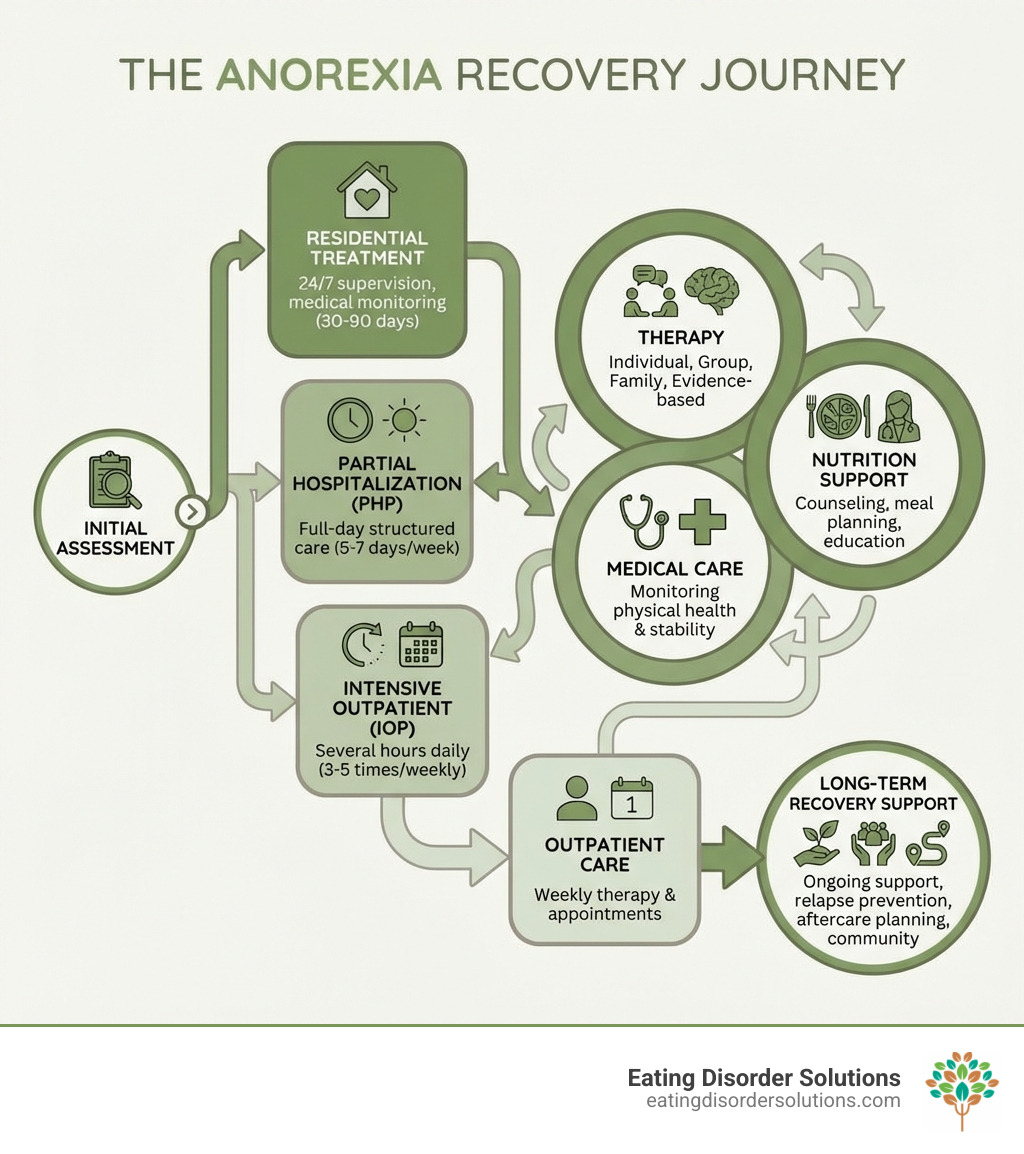
Key Treatment Options at an Anorexia Rehab Center:
- Residential Treatment – 24/7 supervision with medical monitoring, typically 30-90 days
- Partial Hospitalization (PHP) – Full-day structured care, 5-7 days per week
- Intensive Outpatient (IOP) – Several hours per day, 3-5 times weekly
- Outpatient Care – Weekly therapy and medical appointments
- Core Treatment Components – Individual therapy, group therapy, nutrition counseling, medical care, family involvement
If you’re reading this, you or someone you love may be struggling with anorexia. Perhaps you’ve tried to manage it alone, or you’re questioning whether you’re “sick enough” to deserve help. You are.
Anorexia Nervosa is a serious, life-threatening condition that affects your body, mind, and spirit. It thrives in isolation and secrecy. But here’s what matters most: recovery is possible, and you don’t have to face this journey alone.
An anorexia rehab center provides the structured, compassionate environment where healing can begin. These specialized facilities understand that anorexia isn’t just about food—it’s about addressing the underlying thoughts, emotions, and experiences that fuel the disorder.
This guide will walk you through what to expect from anorexia treatment, from understanding warning signs to choosing the right level of care. You’ll learn about the therapeutic approaches that work, how medical and nutritional support happens, and what role your family can play in recovery.
As one former patient shared: “It is difficult to reach out at first, but going to treatment literally saved my life.”
Understanding Anorexia Nervosa and Warning Signs
Anorexia Nervosa is often misunderstood as a “lifestyle choice” or an extreme diet. In reality, it is a complex mental health condition characterized by an intense fear of gaining weight and a distorted perception of body shape or size. We see it every day: individuals who are incredibly high-achieving and capable, yet trapped by a voice that tells them they are never thin enough.
The primary hallmark of anorexia is restrictive eating. This involves limiting calorie intake to the point of significant weight loss or failure to maintain a healthy weight for age and height. However, there is also a binge-eating/purging type of anorexia, where an individual restricts food but also engages in compensatory behaviors like self-induced vomiting or the misuse of laxatives.
It is a common myth that you must be “skinny” to have an eating disorder. This is where Atypical Anorexia Nervosa: Signs & Symptoms come into play. Individuals with atypical anorexia meet all the criteria for anorexia—including the psychological distress and restrictive behaviors—but their weight remains within or even above the “normal” range. The medical risks, including heart failure and electrolyte imbalances, are just as real for these individuals.
Physical and Emotional Warning Signs
Recognizing the signs is the first step toward getting help. If you are unsure, taking an Anorexia Test can be a helpful starting point to evaluate your relationship with food and your body.
Physical Symptoms:
- Rapid or extreme weight loss.
- Dizziness, fainting, or feeling cold all the time.
- Thinning hair or the growth of “lanugo” (fine, downy hair on the body).
- Absence of menstruation (amenorrhea) or irregular cycles.
- Digestive issues like bloating or constipation.
Emotional and Behavioral Changes:
- Preoccupation with calories, ingredients, and “clean” eating.
- Withdrawal from social situations, especially those involving food.
- Intense anxiety about eating in public.
- Excessive or “driven” exercise, often referred to as What is Anorexia Athletica?
- Rigid rituals around food (e.g., cutting food into tiny pieces or eating very slowly).
We also keep a close eye on Orthorexia vs Anorexia. While anorexia is primarily driven by weight and thinness, orthorexia is an obsession with the “purity” or “correctness” of food. Both can lead to severe malnutrition and require professional intervention. For more detailed insights on how these conditions specifically impact women, the Mayo Clinic Women’s Health Information provides excellent resources on the intersection of hormonal health and eating disorders.
Finding the Right Level of Care at an Anorexia Rehab Center
When you decide to enter an anorexia rehab center, the first thing we do is a comprehensive assessment. This isn’t just about your weight; it’s about your heart health, your lab work, your psychiatric history, and your personal goals. Based on this, we determine the “level of care” that will best support your safety and long-term success.
The Continuum of Care
Recovery isn’t a “one size fits all” process. We offer a range of programs designed to meet you where you are:
- Residential Eating Disorder Treatment Program: This is the most intensive level of care we provide in our Texas locations. It offers 24/7 supervision and medical monitoring in a home-like, tranquil environment. This level is ideal for those who need constant support to interrupt disordered behaviors and stabilize their physical health.
- Partial Hospitalization Eating Disorder Treatment Program: Often called “Day Treatment,” PHP allows you to spend the majority of your day (usually 5–7 days a week) in our center for therapy and supervised meals, while returning home or to a supportive living environment at night.
- Intensive Outpatient Eating Disorder Treatment Program: IOP is a step down from PHP. It typically involves several hours of therapy a few days a week. It’s designed to help you transition back into daily life—work, school, or family—while still receiving professional support.
- Outpatient Eating Disorder Treatment Program: This involves weekly sessions with a therapist and dietitian. It is often the final stage of a long-term recovery plan.
Comparison of Care Levels
| Level of Care | Supervision | Medical Monitoring | Typical Schedule |
|---|---|---|---|
| Residential | 24/7 On-site | Daily/Constant | Full-time living on-site |
| PHP | Daytime/Structured | Frequent | 6–8 hours/day, 5–7 days/week |
| IOP | During Sessions | As needed | 3 hours/day, 3–5 days/week |
| Outpatient | Scheduled Sessions | Periodic | 1–2 hours/week |
According to Residential Care Standards, this level of care is specifically designed for those who are medically stable but lack the psychological stability to manage their eating disorder behaviors independently. In our Dallas and Weatherford facilities, we ensure that while the environment is clinical enough to be safe, it feels like a home—not a hospital.
Therapeutic Modalities and Medical Support
At our anorexia rehab center, we believe in treating the whole person. This means our multidisciplinary team—psychiatrists, therapists, dietitians, and nurses—works together to create a unified plan. Anorexia Treatment isn’t just about weight restoration; it’s about rewiring the brain’s response to food and body image.
We utilize the 6 Stages of Our Holistic Eating Disorder Treatment to guide this process. This holistic approach ensures we aren’t just checking boxes, but actually fostering deep, internal change.
Evidence-Based Therapies in an Anorexia Rehab Center
We don’t guess when it comes to your health. We use therapies that have been clinically proven to help, though we tailor them to the specific needs of anorexia recovery.
- Dialectical Behavioral Therapy (DBT): This is incredibly helpful for managing the intense emotions that often come with re-feeding. It teaches mindfulness, distress tolerance, and emotional regulation.
- Exposure and Response Prevention (ERP): This is a “gold standard” for tackling the fear of certain foods. Under the guidance of our team, you’ll gradually face “fear foods” and learn to manage the anxiety without resorting to disordered behaviors.
- Cognitive Behavioral Therapy (CBT): While research suggests that standard CBT (CBT-e) may have limitations for those who are severely underweight, we use adapted versions to help challenge the “eating disorder voice” and the rigid thought patterns associated with anorexia.
- Behavioral Activation: This helps you re-engage with the things that bring you joy—hobbies, friendships, and interests—that the eating disorder may have stripped away.
- Family-Based Treatment (FBT): Especially for our younger clients, FBT (also known as the Maudsley Approach) empowers the family to take an active role in the recovery process.
Medical and Nutritional Support in an Anorexia Rehab Center
You cannot “think” your way out of malnutrition. The brain requires adequate fuel to process therapy effectively. This is why nutritional rehabilitation is the foundation of our program.
- Registered Dietitians: You will work one-on-one with a dietitian who understands the complexities of anorexia. They don’t just hand you a meal plan; they help you understand why your body needs specific nutrients.
- Meal Support: One of the hardest parts of rehab is the actual act of eating. Our staff provides compassionate meal support, sitting with you during meals to offer encouragement and help you use your coping skills in real-time.
- Medical Stabilization: For those in residential care, we monitor electrolytes, heart rate, and blood pressure closely. Refeeding syndrome is a serious risk, and our medical team is trained to manage the transition to regular eating safely.
- Nutrition Education: We move away from “good” vs. “bad” food labels. Instead, we focus on balance, variety, and the social/emotional aspects of eating.
Addressing Co-occurring Disorders and Family Involvement
Rarely does anorexia exist in a vacuum. Most of the individuals we treat are also battling “co-occurring disorders” or a dual diagnosis. This might include:
- Depression: The malnutrition of anorexia often mimics or worsens clinical depression.
- Anxiety and OCD: Many people with anorexia struggle with a need for control and perfectionism.
- Trauma and PTSD: For many, an eating disorder is a way to cope with past trauma. Our Eating Disorder Treatment is trauma-informed, meaning we prioritize your sense of safety and empowerment.
- Substance Use: Sometimes, individuals use substances to suppress appetite or numb the pain of the disorder.
The Role of the Family
We often tell our families: “You didn’t cause this, but you are a vital part of the cure.” Especially for adolescents, we view parents and caregivers as “supportive change makers.”
Family involvement includes:
- Weekly Family Therapy: Addressing the dynamics that may have been strained by the eating disorder.
- Education: Helping loved ones understand that anorexia is a brain-based illness, not a choice.
- Skill Building: Teaching parents how to provide non-judgmental support during meals and how to handle “slips” or setbacks with compassion.
Frequently Asked Questions about Anorexia Rehab
How long does residential treatment usually last?
The average length of stay in a residential anorexia rehab center is between 30 and 90 days. However, there is no “magic number.” Some people may stay longer if they need more time for medical stabilization, while others may step down to PHP or IOP sooner. The goal is clinical stability—when you can manage your meals and emotions with less intensive supervision.
Are antidepressants effective for anorexia?
It is a common question, but the research is clear: antidepressants have not been shown to be effective for people who are significantly underweight. This is because the brain’s chemistry is so altered by malnutrition that the medication cannot work as intended. Once weight restoration has begun, medication may be helpful for treating co-occurring depression or anxiety, but talk therapy and nutritional rehabilitation remain the primary treatments for anorexia itself.
Can I use insurance to pay for rehab?
Yes, most major insurance plans cover eating disorder treatment. We know that the financial aspect can be stressful, which is why we handle the insurance verification process for you. We are in-network with many providers and work hard to ensure you get the maximum benefit available. To understand the process better, you can read more about What to Expect during the admissions and financial planning phase.
Conclusion
Recovery from anorexia is a marathon, not a sprint. It requires a shift in how you view yourself, your body, and the world around you. At Eating Disorder Solutions, we don’t just want to help you “stop the behavior”—we want to help you build a life that you don’t feel the need to escape from.
Our Locations in Dallas, Weatherford, and Ennis, Texas, offer a sanctuary for healing. We provide individualized, compassionate care in a warm, home-like setting because we believe that human connection is the most powerful tool for recovery. We are so confident in our approach that we offer Our Treatment Guarantee: if a client completes our 75-day program and experiences a relapse within one year, they can return for 30 days of treatment at no additional cost.
If you are ready to take that first step, we are here to walk with you. Start Your Recovery Journey today. You deserve a life of freedom, health, and joy. You deserve to be well.









