Understanding When You Need More Than Outpatient Care
Body dysmorphia residential treatment provides intensive, around-the-clock care for individuals whose symptoms have become so severe that outpatient therapy is no longer enough. If you’re spending hours each day obsessing over perceived flaws, avoiding social situations entirely, or experiencing thoughts of self-harm, residential care offers a safe environment where you can focus entirely on healing.
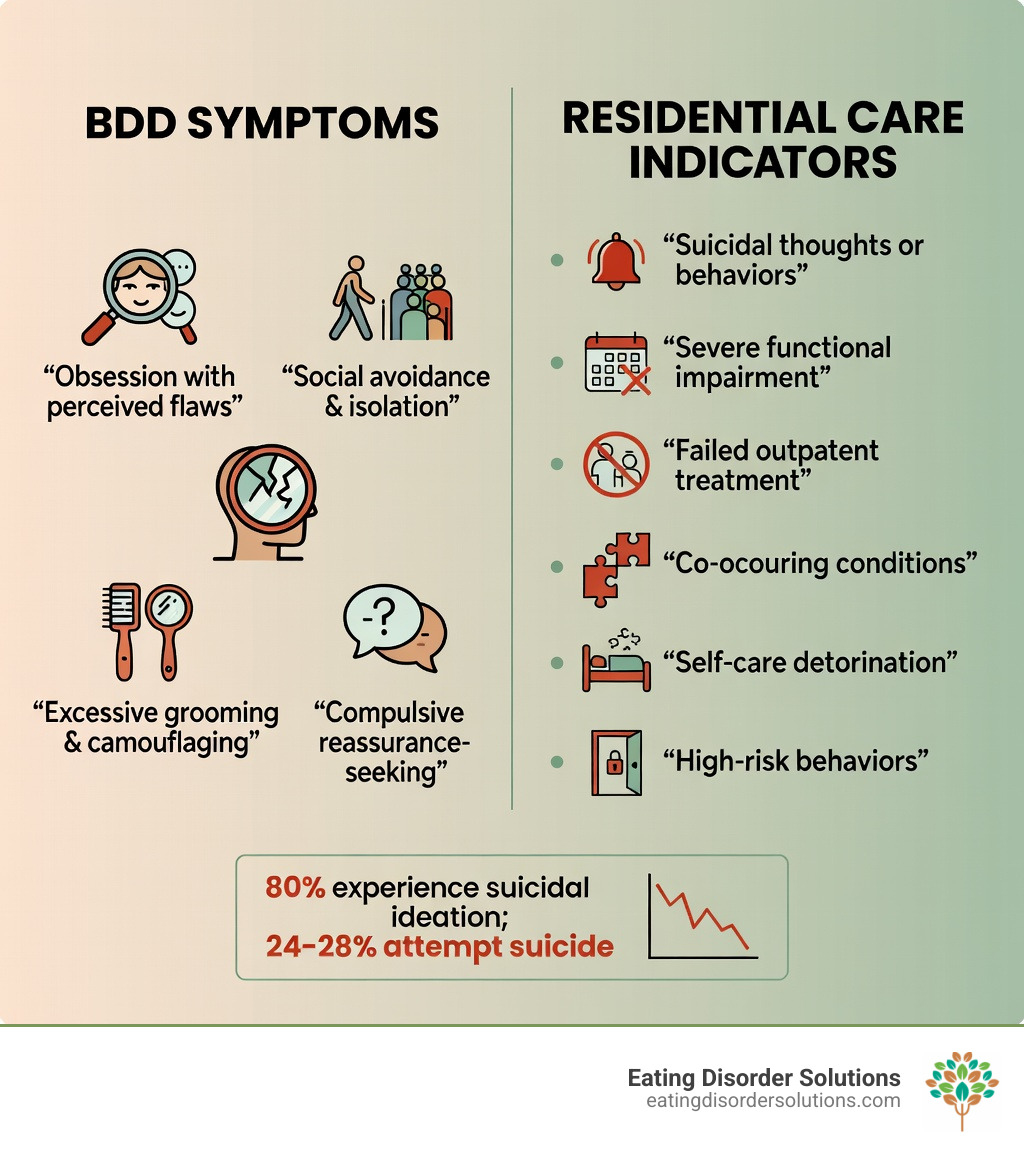
When Residential Treatment is Recommended:
- Suicidal thoughts or behaviors – 80% of people with BDD experience suicidal ideation; 24-28% attempt suicide
- Severe functional impairment – Unable to work, attend school, or maintain relationships
- Failed outpatient treatment – Symptoms persist despite therapy and medication
- Co-occurring conditions – Eating disorders, depression, or substance use alongside BDD
- Self-care deterioration – Cannot manage daily activities independently
- High-risk behaviors – Excessive cosmetic procedures, skin picking, or extreme isolation
Body Dysmorphic Disorder affects 1-2% of the population equally across genders. Unlike typical appearance concerns, BDD involves obsessive preoccupation with perceived flaws that others don’t notice—leading to repetitive behaviors like mirror checking, excessive grooming, or constantly seeking reassurance.
The disorder typically develops in early teenage years but can emerge at any age. Without treatment, it often worsens, creating a downward spiral that impacts every aspect of life. Residential programs interrupt this cycle by removing daily triggers and providing intensive evidence-based care.
Research shows that BDD is frequently misdiagnosed or overlooked, especially in psychiatric settings where it’s “camouflaged” by co-occurring conditions like depression or anxiety. Patients rarely disclose appearance concerns unless specifically asked—making specialized residential assessment crucial for accurate diagnosis and effective treatment.
When is Body Dysmorphia Residential Treatment Necessary?
Deciding to enter body dysmorphia residential treatment is a major life step, but for many, it is the turning point that saves their life. While outpatient therapy is a wonderful tool for mild to moderate cases, BDD has a way of expanding until it consumes a person’s entire day. When the “noise” of the obsession becomes louder than the voice of reason, a higher level of care is required.
Residential treatment becomes necessary when the symptoms move beyond “distressing” and into “dangerous.” Statistics indicate that the annual rate of completed suicide in patients with BDD is 0.3%, which is significantly higher than most other mental health disorders. This highlights the urgent need for a secure, clinical environment when safety becomes a concern.
At Eating Disorder Solutions, we recognize that BDD is not just “vanity” run amok. It is a debilitating obsessive-compulsive related disorder that creates a profound disconnect between reality and perception. When a person can no longer function in their daily life—missing work, failing classes, or refusing to leave the house for weeks at a time—the structured support of a residential facility provides the necessary “pause button” to reset and begin intensive healing.

Identifying Severe BDD Symptoms
Identifying when BDD has reached a critical stage involves looking at the frequency and intensity of compulsive behaviors. While most people have moments of insecurity, individuals requiring body dysmorphia residential treatment often engage in:
- Excessive Mirror Checking or Avoidance: Spending several hours a day analyzing a perceived flaw in the mirror, or conversely, covering all mirrors in the home to avoid the “shame” of their reflection.
- Compulsive Skin Picking: Attempting to “fix” perceived skin irregularities, often leading to permanent scarring or infections.
- Extreme Social Isolation: Avoiding all social gatherings, including work or family events, out of fear that others will notice and judge the perceived defect.
- Seeking Reassurance and Comparisons: Constantly asking loved ones if they look “okay” or spending hours on social media comparing their features to others, which only fuels the cycle of dissatisfaction.
- Cosmetic Procedure Dissatisfaction: A history of seeking dermatological or surgical “fixes” that never provide relief, often leading to increased distress post-procedure.
Clinical Criteria for Inpatient Admission
Clinicians use specific markers to determine if a patient requires the 24/7 monitoring provided by a residential or inpatient setting. According to research on BDD prevalence, BDD is found in approximately 7% of psychiatric inpatient settings, suggesting that many people reaching a crisis point have this underlying condition.
The primary criteria for admission include:
- Psychiatric Stabilization: If a patient is in an active crisis, experiencing hallucinations (though rare in BDD, they can occur in the form of delusional intensity), or severe panic attacks that prevent them from eating or sleeping.
- Self-Care Deficit: When the obsession becomes so time-consuming (often 3 to 8 hours a day) that the individual neglects basic hygiene, nutrition, or medical needs.
- Treatment Resistance: If a person has tried multiple rounds of outpatient therapy or medication without success, a residential program offers a more “concentrated” dose of therapy to break through the resistance.
- 24/7 Monitoring for Safety: For those at high risk of self-harm or suicide, the constant presence of nursing staff and therapists ensures a safety net that outpatient care simply cannot match.
Evidence-Based Therapies and Clinical Interventions
The core of effective body dysmorphia residential treatment lies in evidence-based modalities that retrain the brain’s processing of visual information and emotional responses. At Eating Disorder Solutions, we utilize a trauma-informed care approach, acknowledging that many body image struggles are rooted in past experiences of shame or rejection.
Our clinical interventions focus on two primary goals: reducing the intensity of the obsessive thoughts and breaking the cycle of compulsive behaviors.
Cognitive Behavioral Therapy (CBT) and Exposure and Response Prevention (ERP)
CBT is considered the gold standard for BDD treatment. It helps patients identify the “cognitive distortions”—the lies the brain tells them about their appearance—and replace them with more neutral, realistic thoughts.
A specific type of CBT called Exposure and Response Prevention (ERP) is particularly effective. In ERP, we slowly and safely expose patients to their triggers (like looking in a mirror or going into a public space) while teaching them to resist the urge to perform a compulsion (like applying heavy makeup or checking their reflection). Over time, this “habituation” reduces the anxiety associated with the perceived flaw.
Other therapeutic modalities often included in a comprehensive program are:
- Dialectical Behavior Therapy (DBT): To help with emotional regulation and distress tolerance.
- Acceptance and Commitment Therapy (ACT): Focusing on living a value-driven life despite the presence of difficult thoughts.
- Group Therapy: Providing a space to realize they are not alone and to practice social skills in a safe environment.
Psychopharmacology and Medication Management
While therapy is the cornerstone of recovery, medication can be a vital “crutch” to help lower the baseline of anxiety and obsessive thinking. Scientific research on BDD pharmacotherapy highlights the effectiveness of Selective Serotonin Reuptake Inhibitors (SSRIs).
In a residential setting, psychiatrists can closely monitor a patient’s response to medication, adjusting dosages in real-time to ensure the best results with the fewest side effects. These medications don’t “fix” the perceived flaw, but they do quiet the obsessive thoughts enough to make therapy more effective.
Holistic and Adjunctive Therapies
We believe that true recovery involves the whole person—mind, body, and spirit. Our holistic treatment stages incorporate adjunctive therapies that help patients reconnect with their bodies in a positive, non-judgmental way.
These may include:
- Mindfulness and Meditation: Learning to observe thoughts without reacting to them.
- Art Therapy: Expressing internal pain and perception through creative outlets.
- Yoga and Movement: Gently moving the body to foster a sense of gratitude for what the body can do rather than just how it looks.
- Nutritional Counseling: Ensuring the body is properly fueled, especially if BDD has led to restrictive eating patterns.
Addressing Co-occurring Disorders and Suicidality
It is rare for BDD to exist in a vacuum. On average, patients with BDD present with 2.5 comorbid conditions. This complexity is why body dysmorphia residential treatment is so valuable; it allows a multidisciplinary team to treat all facets of a person’s mental health simultaneously.
The most common co-occurring conditions include:
- Major Depressive Disorder (75%): The isolation and shame of BDD often lead to deep depression.
- Social Anxiety Disorder (40%): A natural byproduct of fearing judgment from others.
- Substance Use Disorders (30-50%): Many individuals use alcohol or drugs to “numb” the pain of their obsessions.
- Obsessive-Compulsive Disorder (33%): BDD is a “cousin” to OCD, and many share the same underlying brain chemistry.
The Link Between BDD and Eating Disorders
There is a significant overlap between BDD and eating disorders. In fact, 32% of individuals with BDD will be diagnosed with an eating disorder at some point in their lives. While both involve body dissatisfaction, the focus differs: eating disorders generally center on weight and overall shape, whereas BDD focuses on specific features like the nose, skin, or hair.
| Feature | Body Dysmorphic Disorder (BDD) | Eating Disorders (Anorexia/Bulimia) |
|---|---|---|
| Primary Focus | Specific body part (e.g., facial features, skin, hair) | Overall weight, shape, and body size |
| Compulsive Behaviors | Mirror checking, grooming, skin picking | Calorie counting, purging, excessive exercise |
| Gender Distribution | Affects men and women almost equally | Historically higher in women, but increasing in men |
| Repetitive Acts | Comparing appearance to others | Frequent weighing, body checking |
At Eating Disorder Solutions, we specialize in treating the intersection of BDD and eating disorders. We understand that a patient might be restricting food not just to lose weight, but because they believe a thinner face will hide a perceived “defect” in their jawline.
Managing High-Risk Behaviors
Safety is our absolute priority. Because of the high rates of suicidality associated with BDD, our residential facilities in Dallas and Weatherford provide 24/7 nursing support and crisis intervention.
We focus on:
- Safety Planning: Helping patients identify their triggers and develop a “toolbox” of coping skills to use when they feel overwhelmed.
- Behavior Interruption: Gently stopping compulsive behaviors like skin picking or mirror checking before they escalate.
- Trauma-Informed Support: Providing a compassionate environment where patients feel safe enough to share their darkest thoughts without fear of judgment.
Frequently Asked Questions
How long does body dysmorphia residential treatment last?
The length of stay is highly individualized. While the average stay in a residential program ranges from 30 to 90 days, we focus on progress rather than a specific calendar date. Some individuals may require a longer stay to achieve stability, while others may transition to a partial hospitalization program (PHP) sooner.
To help you feel more comfortable about the process, we provide detailed information on what to expect during your time with us, from the intake process to daily schedules.
What are the goals of body dysmorphia residential treatment?
The ultimate goal is functional recovery. This means more than just “liking” how you look; it means reaching a place where your appearance no longer dictates your happiness or your ability to participate in life.
Specific goals include:
- Reducing the time spent on obsessions and compulsions.
- Developing healthy coping mechanisms for distress.
- Improving social and occupational functioning.
- Building a foundation of self-acceptance and body neutrality.
Is family involvement part of the recovery process?
Absolutely. BDD doesn’t just affect the individual; it affects the entire family unit. Loved ones often feel helpless, frustrated, or may inadvertently “enable” the disorder by providing constant reassurance.
We incorporate family therapy and education into our programs to help your support system understand the nature of BDD. We also work closely on aftercare planning to ensure that the progress made in treatment is maintained once you return home.
Conclusion
Recovery from Body Dysmorphic Disorder is not about achieving “perfection”—it is about achieving freedom. Freedom from the mirror, freedom from the shame, and freedom to live a life that is no longer defined by a perceived flaw.
At Eating Disorder Solutions, we provide a warm, home-like setting in Dallas and Weatherford, TX, where you are treated as a human being, not just a diagnosis. Our holistic, trauma-informed approach is designed to meet you where you are and guide you toward self-acceptance. We are so confident in our individualized care that we offer a 75-day treatment guarantee—if you complete our program and meet the criteria but experience a relapse, you can return for additional support.
If you or a loved one are struggling, don’t wait for the cycle to get worse. Reach out to our admissions team today to learn more about how we can help.
Start your journey toward healing today with our specialized body dysmorphic eating disorder treatment. You deserve to see yourself through a lens of compassion and truth.








